Spinal arachnoid adhesion
It is rare. As of 2021, less than 50 cases have been described (according to Greenberg MS. Handbook of Neurosurgery. 10th ed.; 2023). It is slightly more common in men. In all cases, adhesions are described at the thoracic level – in the vast majority of cases between the 2nd and 8th thoracic vertebrae. In 95% of cases, it is located on the posterior surface of the spinal cord .
What are the possible reasons?
Infectious diseases, subarachnoid hemorrhages, trauma, and others.
What is it manifested by?
Pain in the thoracic spine. Later, symptoms appear in the lower extremities, and then myelopathy – that is, a decrease in strength in the lower extremities, impaired sensitivity in them, impaired function of the pelvic organs. Numbness and paresthesia in the upper extremities are not uncommon.
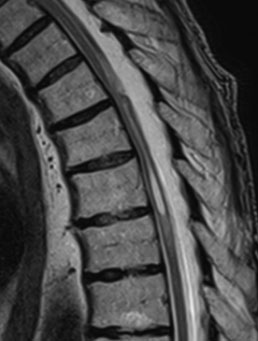
The main diagnostic method is MRI, which reveals spinal cord displacement and a “scalpel” compression zone. It also reveals a zone of myelopathy (a zone of spinal cord edema).
Treatment is surgical only. During the operation, access to the spinal cord is made , and then the adhesion is detected and completely excised along with the places of adhesion to the surrounding structures. An audit of the surrounding structures is performed to confirm the patency of the cerebrospinal fluid pathways.
In the postoperative period, symptoms of spinal cord injury usually regress well.
The operation for such an arachnoid adhesion was performed at the KNP TOKPNL TOR. The 71-year-old patient had pronounced lower paraparesis for 4 years, which gradually increased. 4 weeks before admission, he stopped walking. At the same time, his legs involuntarily moved sharply, as if “jumping”, even in his sleep, which prevented him from sleeping. This condition is called spasticity. It occurs due to the loss of control over spinal reflexes from the brain . The patient could sit in bed only with help, or “by supporting himself with pillows on all sides”. The strength of the trunk muscles was no longer enough for such ordinary things. A few days before the operation, control over the functions of the bladder and intestines disappeared. Doctors had to install a urinary catheter. A typical “scalpel symptom” was detected on MRI.
We are talking about a posterior pathology – arachnoid membrane. A 71-year-old patient with diabetes mellitus has had progressive low paraparesis for 4 years. He has been unable to walk for the last 4 weeks.
The situation was complicated by severe diabetes mellitus, which could increase the risk of postoperative complications. However, the decision to operate was made and the operation was performed through a minimally invasive approach – that is, through a tube 2.5 cm in diameter, which was installed on the right in the projection of the fifth thoracic vertebra, where the adhesion was found on the MRI. A hemilaminectomy was performed – that is, only half of the vertebral arch was removed, while usually in such operations the arches are removed completely and at 2-3 adjacent levels. Such a careful attitude to the tissues and structures of the spine allows to reduce the need for additional fixation of the spine with metal structures. Tissue trauma is also reduced, which reduces the risk of complications, especially in diabetes mellitus. And after opening the dura mater of the spinal cord, the adhesion itself was detected. It was possible to completely remove it, which can be seen in the video .
Immediately after the operation, the restoration of functions began. First of all, control over the bladder was restored. The catheter was removed. Then, spasticity in the lower extremities gradually decreased and the level of control increased. A 71-year-old man, who had not been able to even sit in bed for a long time, began to sit up, and soon to get out of bed. The joy of the family and the patient himself knew no bounds. And together with him, the doctors and the entire team of the neurosurgical department of the KNP TOKPNL TOR rejoiced.
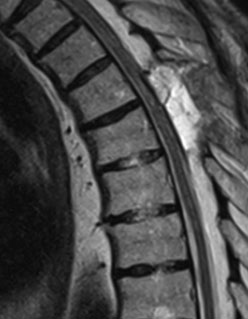
MRI control after surgery is good. The area of myelopathy has decreased and become less intense.
The patient was treated by the head of the neurosurgery department , Oleksiy Leontiev , and neurosurgeon Vyacheslav Dmytruk.
Prepared by Alexey Leontiev
Leave a Reply